What If I Find Out That I Am Group B Strep Positive?
So you have been riding the waves of early pregnancy and all things seem to be going quite smoothly. Next thing you know, you get the results back from a test you had done a month ago and you find out you are Group B Strep positive, what is next? Hopefully you will find this blog post helpful when navigating all things Group B Strep so please do read on.

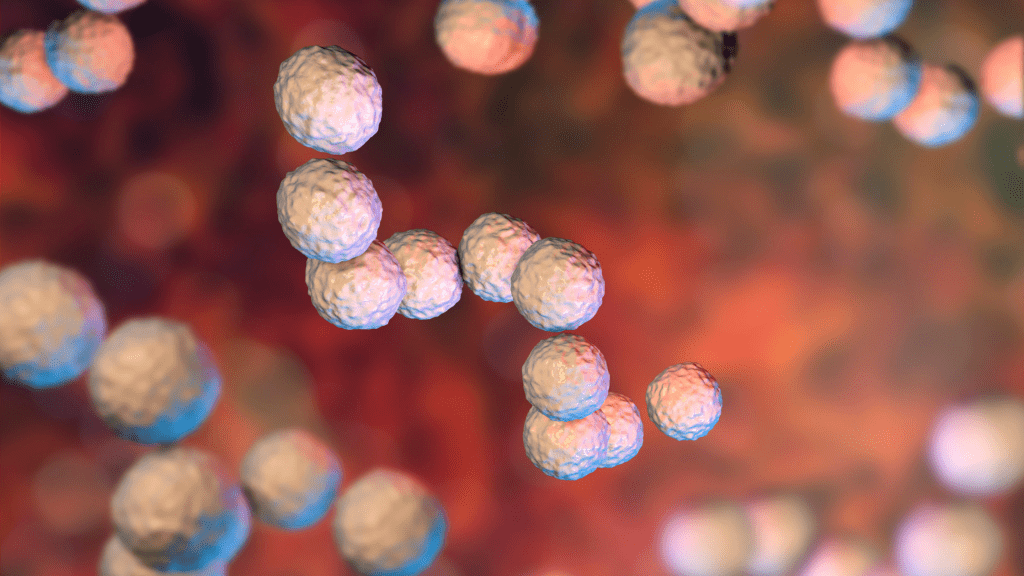
What Is Group B Strep?
Group B Strep / Streptococcus or Streptococcus Agalactiae is a bacterium that actually forms part of the normal flora of the human gut. This basically means that it lives within the human gut of plenty of men and women and the lower vaginal tract of women accordingly, without causing harm or disease.
Group B Strep is estimated to be present in the vagina and rectum of 2 – 4 in 10 women in the UK. Group B Strep does not usually cause symptoms however some women can experience symptoms if it is present in their urinary tract.
In This Case How Is Group B Strep A Problem?
We can accept that Group B Strep generally is not a problem for the mother but how and why is it a problem for babies?
Firstly babies have immature immune systems making it harder for them to fight off infection. This essentially becomes more of a problem the younger or the more premature a baby is. Secondly if a baby was to come into contact with Group B Strep it would likely make an entrance into the baby via somewhere where it does not form part of the normal flora i.e the lungs.
Very rarely does a baby become infected with Group B Strep whilst in the womb as the membranes and amniotic fluid around the baby form an effective barrier against this. But if and once the membranes have broken and released amniotic fluid, this effective barrier is compromised and Group B Strep, if present in the vaginal tract can now reach and cause illness in the baby.

Is There Anything That Increases The Chances Of A Baby Becoming Unwell With Group B Strep?
- Mother testing positive for Group B Strep
- Previous baby unwell from Group B Strep infection
- Preterm baby (less than 37 weeks gestation at birth)
- Maternal raised temperature or signs of infection in labour
- Membranes broken more than 24 hours before baby is born
What Could Group B Strep Mean To A Baby?
It is fair to assume that many babies come into contact with Group B Strep during labour and or birth, and most of these babies do not become unwell as a result of this exposure.
An average of 43 babies a month (uk based numbers) develop an early onset Group B Strep infection where they become unwell as a result of the bacterium within the first week of their lives. (Late onset Group B Strep in the first 3 months of life is considered separately as antibiotic administration in labour has no benefit against this subset of the illness).
Of these 43 babies an average of 38 make a full recovery, 3 survive but with long-term mental and or physical disabilities and sadly an average of 2 die as a result of the infection.
These numbers do highlight that treatment for babies who become unwell with Group B Strep is highly effective, this may be relevant or important for some when deciding what to do following detection of Group B Strep in pregnancy.
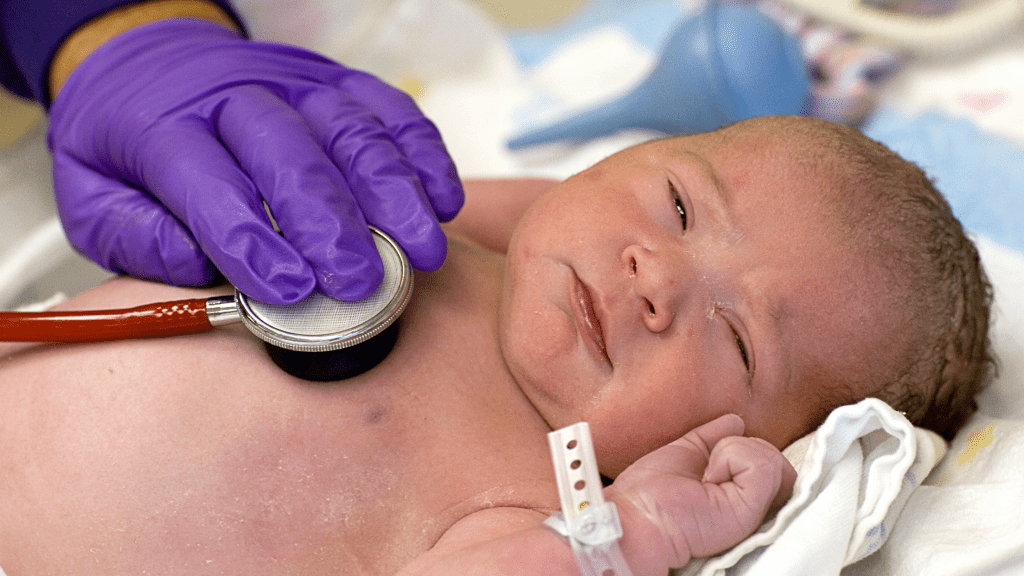
How Are Babies Monitored For Group B Strep Infection?
If someone who tested positive for Group B Strep in pregnancy, decides to opt for antibiotics in labour and receives it in a timely and appropriate manner then no monitoring of their baby is considered necessary.
If someone declined antibiotics or received them less than 4 hours before they birthed, the recommendation is that their baby receives regular assessments of general wellbeing for the first 12 hours of their life. After this, and if they have remained well then the chances of their baby becoming unwell from Group B Strep is considered very low.
For anyone who had a previous baby who became unwell from Group B Strep, even if they received antibiotics based on recommendations, it is still considered most safe to have their baby receive regular assessments of wellbeing for the first 12 hours of their life also.
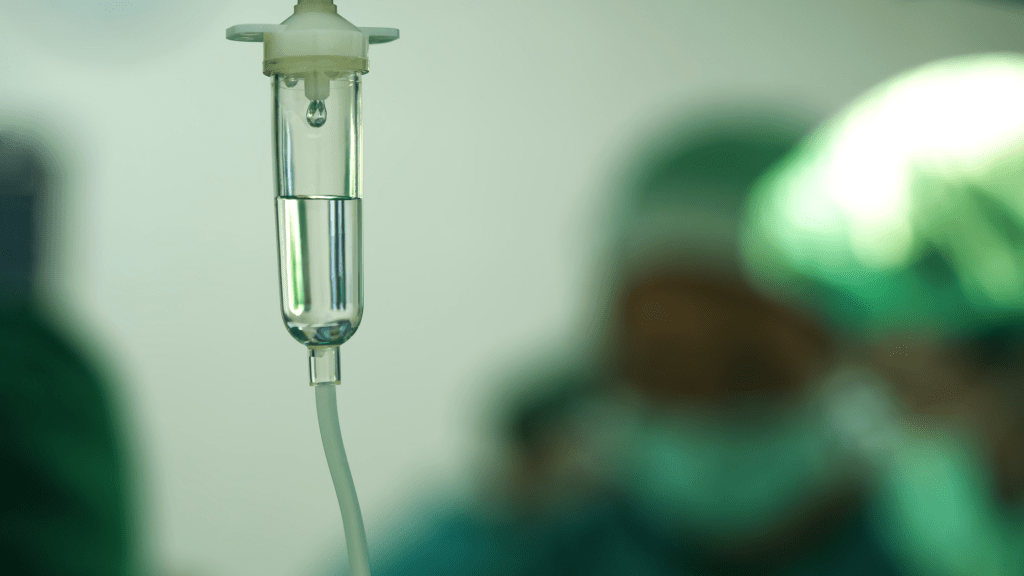
Is There Anything More To Think About Here?
A problem commonly encountered around administration of antibiotics is with the timing of administration and how this is facilitated or guaranteed within the NHS in particular. This is something that needs to be factored into decision making around Group B Strep. Evidence suggests that unless antibiotics are given 4 hours or more prior to birth of the baby then they are not considered as effective. As a result the same length and level of observations for babies born in this situation are recommended after birth, before they are considered to have lower chances of developing an early onset Group B Strep infection if they remain well.
Further difficulty lies with deciding on when to start intravenous antibiotics. When is too soon or too late? How long until someone’s labour starts? How easy is the person to cannulate? Who is available to cannulate? Is anyone free to check intravenous drugs ready for administration? When is this convenient to the woman? All of these things need careful consideration as they may impact on when antibiotics are administered and therefore how effective they are.
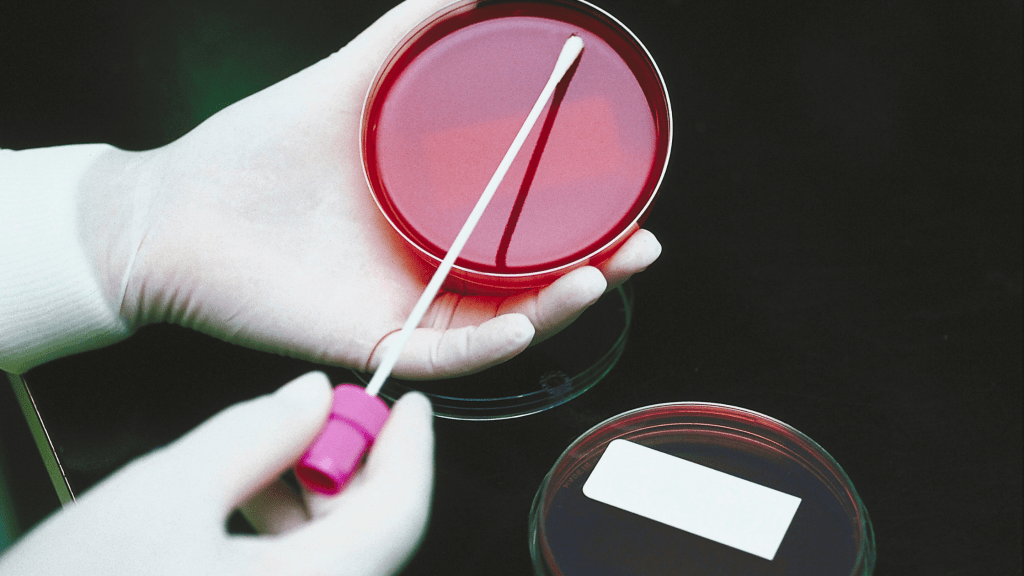
How Is Group B Strep Detected?
Group B Strep can be detected via traditional microbiological laboratory testing particularly through the standard direct plating method. This involves swabbing the lower vagina and the rectum, incubation of the sample on some agar growth medium and then identification or not of Group B Strep. This method usually yields results within 4 – 5 days give or take. It is also important to note that this traditional form of testing actually has around a 50% false negative result, so half of women tested for Group B Strep using this method are told they do not have Group B Strep at the time of testing when they do.
Another form of Group B Strep testing is called Sensitive Enriched Culture Medium (ECM) Testing. It is readily available privately however not widely available on the NHS (some trusts do offer this form of testing), I would imagine this is mostly due to it being more costly. It has a clear benefit of a quicker turnaround of results (by 2-3 days compared to traditional testing) alongside increased sensitivity and accuracy.
The other possible test is a polymerase chain reaction test, with a similar sensitivity to an ECM test, and very rapid results, the only downfall being it requires expensive equipment and therefore is not really used for this purpose and definitely not in the NHS.
Should And How Can Group B Strep Be Treated?
When detected in the mother, during pregnancy, Group B Strep is not treated (except if detected in urine especially if symptoms of a urinary tract infection are present), it is simply carefully noted for future reference. Current recommendations are that if Group B Strep has been detected at any stage of a current pregnancy or in a previous pregnancy, once labour commences or if membranes break, antibiotics should be commenced as soon as possible.
Why These Recommendations For Group B Strep?
So, when Group B Strep is detected in pregnancy for the first time, intravenous antibiotics in labour is recommended. The rationale behind this recommendation is as outlined previously in this blog, and mostly due to babies’ immune systems being immature.
As for the previous pregnancies where Group B Strep was detected, more information and consideration is best…
The first thing to consider here is whether or not the baby in the previous pregnancy, born to the mother who tested positive for Group B Strep, was affected or developed illness as a result of Group B Strep or not. If the baby was unaffected, evidence suggests that there is a 1 in 2 chance that Group B Strep might be present in the mother in subsequent pregnancies and the recommendation is actually to opt for an ECM test between 35 and 37 weeks of pregnancy to be able to better decide what to do.
What If The ECM Test Comes Back As Negative?
If the ECM test is negative then the chances of the baby becoming unwell from Group B Strep early on after birth can be as low as 1 in 5000. For some this justifies not using antibiotics in labour but obviously some will still opt for it, it is a matter of personal choice.

What If The ECM Test Comes Back As Positive?
If the ECM test is positive at this stage, then the chances of the baby becoming unwell from Group B Strep early on after birth is considered to be much higher, in fact as high as 1 in 400 and the recommendation remains to be administration of intravenous antibiotics in labour.
Surely It Is A No Brainer? Group B Strep Positive = Antibiotics
Currently the focus for avoiding illness in babies as a result of Group B Strep does indeed lie with antibiotics. Though receiving antibiotics may seem a simple win – win decision, for many it is not an easy one. Antibiotics do come with side effects and implications which extend to the baby also, such as the health and wealth of their fragile microbiomes or normal floras. And to make decision making around this harder, Group B Strep is considered a transient bacteria, meaning one time it may be present in someone’s body and another time not, with no control over or way of predicting when or how.
The turnaround time for traditional Group B Strep testing is another problem. If someone has Group B Strep detected at say 15 weeks of pregnancy and they wanted to find out if they have it once their labour started, the results would not likely be back in time for the results to be used to inform a decision around receiving antibiotics or not.

So does the power lie with Enriched Culture Medium testing and resting decisions on this?
Or does the power lie with a fully informed and supported, autonomous decision? (Maybe even including an ECM test…) I will let you be the judge of this!
Learn more about antenatal midwifery care and support and what is available to you through The Nurture Mama Ltd, by clicking on the following link https://thenurturemama.co.uk/antenatal/. I am currently working on future services I will be offering for support with decision making, so please stay tuned.
Now to finish with a quote by Sara Wickham, it summarises Group B Strep and decision making around this concisely.
‘The chance of Group B Strep disease is very small. The consequences can be serious.
It is always a good idea to get informed before you decide what’s right for you’.
– Sara Wickham
For more info on this topic, why not visit any of the following website pages:
https://www.groupbstreptest.co.uk/why-is-group-b-streptococcus-a-concern/
Or if you enjoy reading books then have a look at the following book which you may find helpful when exploring the topic of Group B Strep in pregnancy
Did you enjoy or find this blog post useful? Why not share it on your social media.
The Nurture Mama Ltd is a fully insured (through ZEST Health Innovation Consultancy Ltd), independent midwife service that offers Antenatal, Postnatal, Combined and Complete packages. Caring, supporting and empowering people throughout pregnancy, labour, childbirth and after birth – giving families complete continuity of care.